Is an enthusiastic and open minded writer. She believes in…
World Sickle Cell Day was established by the United Nations General Assembly in 2008 to increase awareness about this genetic disorder that can be cured and managed if diagnosed early. The day is marked on the 19th of June every year.
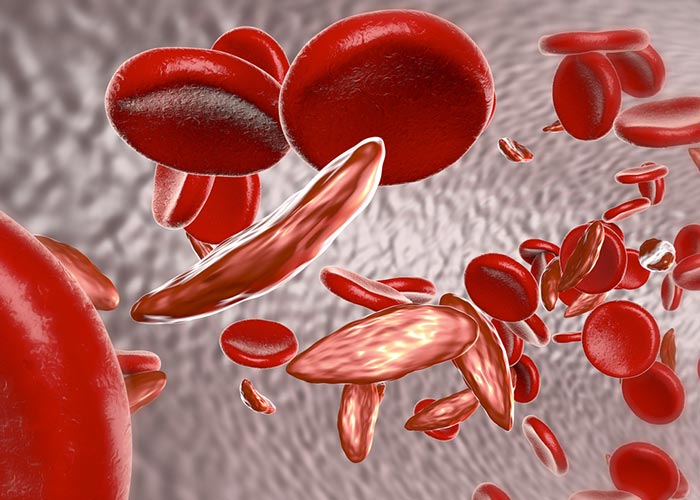
Sickle cell disease is an inherited blood disorder that can be acquired from either or both the parents. The irregular shaped Red Blood Cells (RBCs) in this condition get stuck in the small blood vessels and slow down or block the blood flow and oxygen to various parts of the body. Imaginably, it is a painful disease and while there is no cure yet for sickle cell anaemia, certain treatments can help relieve the pain and avoid ailments associated with this disorder.
A healthy person has spherical red blood cells, but one suffering from Sickle Cell Disease (SCD) will have rigid, sticky and crescent-shaped, sickle-like red blood cells (RBCs).
Although this year brings a bit of good news regarding the drug pipeline for sickle cell disease, pain management is a growing problem.
What are the symptoms?
* Patients can develop low haemoglobin, requiring transfusions.
* They can also develop periodic episodes of pain, called crises starting from the first year of life, which can be very disabling.
* Such patients are also prone to developing repeated pneumonia, painful swelling of hands and feet, sudden enlargement of the spleen (an organ that fights infection), stroke, vision problems, delayed growth and other complications of the bone.
What are the causes?
It is an inherited disorder and even if one of the parents has it, the child is susceptible to the disease and may have one normal haemoglobin gene and one defective form of the gene. Thus, their bodies will produce both normal and sickle cell haemoglobin. However, if both the parents have an affected gene, then the child will have the disease too.
What are the precautions one can take?
* Dehydration and lack of oxygen must be avoided.
* Patients must remain hydrated at all times and should take extra care if they are travelling to higher altitudes.
* Patients affected by the disease should follow up with haematologists on regular basis.
What is the treatment available?
* Patients with this condition should have additional folic acid and protection from pneumonia in the form of a vaccine and antibiotic prophylaxis.
* Hydroxyurea can significantly benefit patients suffering from this disease in reducing or eliminating the requirement for blood transfusion, reduction in painful episodes and decrease in the risk of stroke and other complications associated with the disease.
* The only curative treatment of the disease is Allogeneic Bone Marrow Transplant, which has a very high success rate. If there is Human Leukocyte Antigen (HLA) matched donor in the family, then that donor is preferred the most. However, if there is no matched family donor, a potential donor can be searched from the Bone Marrow Donor Registries. This is referred to as Matched Unrelated Donor transplant.
* Currently, newborn screening programs have been initiated in certain parts of India, so that affected babies can be identified early and appropriate treatment can be started. If there is an affected child in a family, it is possible to check for this condition in the next pregnancy so that the family has the option of terminating the pregnancy.
Is an enthusiastic and open minded writer. She believes in excellence and is always willing to lend her voice to necessary courses that are dear to her heart. Jewel is also a content developer and an upcoming media strategist.